Stories and Successes |
|
4/6/2020 1 Comment Tobacco & Your petsAs you may know, tomorrow is National Pet Day! And I know that you do not need me to tell you about the harmful affects that smoking can have on your own health, or even the harmful affects that second-hand smoking can have on the individuals that you live with, but it is rare that we have the opportunity to talk about the affect that tobacco use can have on the animals that live in your home. Because our pets share our environments, they also share our environmental exposures. Second-hand smoke does affect the health of the animals that are living in the home of a smoker. Dogs living in homes with smokers have significantly higher levels of cotinine (a breakdown product of nicotine) in their blood, indicating exposure to secondhand smoke. Dogs were also more than twice as likely to develop lung cancer if a smoker lived in the home. Also, cats that live in smoking households are more than twice as likely to develop malignant lymphoma (a type of cancer) compared to cats in nonsmoking households. Smoking outside the home reduces the concentration of environmental tobacco smoke in the house, but doesn’t eliminate it. A study found that environmental tobacco levels in homes of smokers who smoked outdoors were still five to seven times higher than in households of nonsmokers. And it’s not just the secondhand smoke that poses a risk for your pets: discarded cigarette butts or other tobacco products left within reach of pets can cause gastrointestinal problems or even nicotine toxicity if your pet finds and eats them. If you choose to use cigarettes or e-cigarettes, please consider quitting not just for the sake of your own health, but for the health of your family and your pets. And if you choose to use these products, make sure to take extra precautions to keep your pets safe.
1 Comment
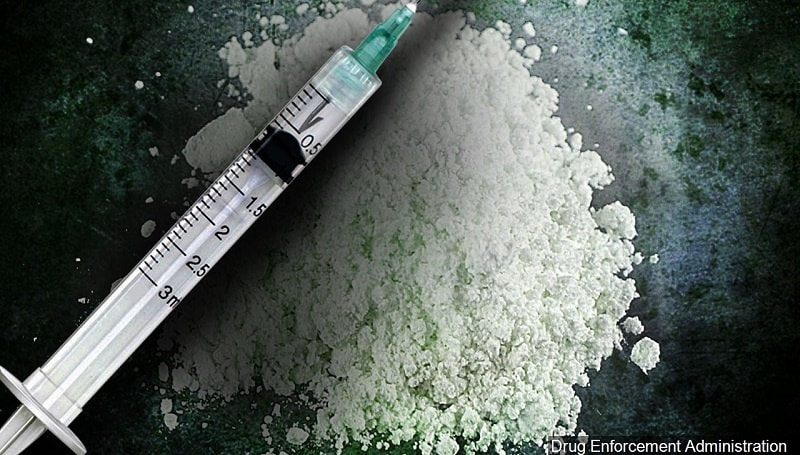
Overdose deaths have increased across the country over the last couple of years, but Hancock County in Indiana is choosing to combat the problem in a new, and controversial, way.
In an article in the Indy Star, they lay out the size of the problem in Hancock County: “According to Indiana State Department of Health data, there were 84 opioid-related emergency department visits and 11 hospitalizations in Hancock County in 2018, the most recent data available.” Hancock County’s prosecutor, Brent Eaton, played a big part in making changes to the way they approach addiction and overdose. These changes include bringing charges against people who overdose in the county. While Eaton says he struggled with this decision, he told Fox 59 News the goal is to “[s]top that revolving door of people that would overdose that we would respond, they go to the hospital and then they go back out to the same environment.” This means that people who overdose in Hancock County will face charges of Possession of a Controlled Substance, which is a Level 6 Felony and could result in a jail sentence between six months and two-and-a-half years. Fox 59 News reports that, after the person is sent to the hospital to treat the overdose, “officers will fill out a form to determine if there is probable cause to file charges.” The person who has overdosed is given the opportunity to plead guilty, and if they go that route, “the prosecutor’s office would agree to offer treatment services through probation,” instead of arresting the person and making them serve jail time. When faced with questions as to whether or not this is a good idea, Eaton told Fox 59 News, “We are enforcing the laws in the State of Indiana. It is against the law to possess controlled substances. That is the law the legislature passed. People in this community, we do not want anyone else to die. We don’t want that to happen.” Criminal defense attorney Bill Frederick told the Indy Star that this new protocol in Hancock County is something that isn’t seen being used very often. “… the practice of charging a person with possession based on the drug being found in their system is unusual. But because state law isn’t explicit about what possession means, it could conceivably hold up in court.” In the past, prosecutor had to rely on actually finding the drug or paraphernalia at the scene of an overdose. Critics of the new course of action are afraid that criminalizing overdoses means more people will die, because those around the overdosed person will be afraid to call 911. They’re also worried that this new action will saddle people with felony charges for years to come, even after they’ve gotten sober. One of this plan’s critics is Reg McCutcheon who works as the executive director of Landmark Recovery in Carmel. McCutcheon was recently interviewed by WTHR, where he voiced his concern with criminalizing overdoses. McCutcheon told WTHR that addiction “is a disease and we’re criminalizing the disease side and that’s what we have to be mindful of. Statistics do not support forcing someone [into treatment]. We have a national average in excess of eight times before [those struggling with addiction] they find ways to get help.” The executive director of the Hall Center for Law and Health at Indiana University’s Robert H. McKinney School of Law, Nicolas Terry, is also concerned about how Hancock County is choosing to combat addiction and overdose. He recently told the Indy Star that this “new protocol sends a dangerous message, particularly around the use of Naloxone. Since the use of the overdose reversal drug can be used as evidence of opioid use and ultimately drug possession.” Terry added that these fears surrounding Naloxone might mean that fewer people will choose to possess the life-saving drug, fearing that they could be arrested and charged. Prosecutor Eaton told the Indy Star that simply having Naloxone is not a reason to charge someone with possession of a controlled substance, but he also said it’s an indicator that someone has opiates in their system, which can tip off authorities. Nicolas Terry thinks this type of approach will erode “trust between drug users and first responders, and could prevent people from calling 911.” It should be interesting to see how this new protocol will affect the people of Hancock County, and as we start seeing results, we will bring you those updates. 1/6/2020 0 Comments Teen-Vaping on the riseNIH’s 2019 Monitoring the Future survey finds continuing declines in prescription opioid misuse, tobacco cigarettes, and alcohol
Findings from the 2019 Monitoring the Future (MTF) survey demonstrate the appeal of vaping to teens, as seen in the increased prevalence of marijuana use as well as nicotine vaping. Results from the 45th annual MTF survey, a nationally representative sample of eighth, 10th and 12th graders in hundreds of U.S. schools, were announced today by the director of the National Institute on Drug Abuse (NIDA), part of the National Institutes of Health, along with the University of Michigan scientist who leads the research team. The self-report survey is given annually to students who respond to questions about their drug use and attitudes. Past year vaping of marijuana, which has more than doubled in the past two years, was reported at 20.8% among 12th graders, with 10th graders not far behind at 19.4% and eighth graders at 7.0%. Past month marijuana vaping among 12th graders nearly doubled in a single year to 14% from 7.5%–the second largest one-year jump ever tracked for any substance in the history of the survey. (The largest was from 2017-2018 with past month nicotine vaping among 12th graders). For the first time, the survey measured daily marijuana vaping, which was reported at 3.5% among 12th graders, 3.0% among 10th graders, and 0.8% among eighth graders. The MTF investigators documented more detailed findings on teen vaping of marijuana in a research letter released today in the Journal of the American Medical Association. High rates of nicotine vaping reported in the MTF survey were released in September. Marijuana continues to be the most commonly used illicit drug by adolescents. After remaining mostly stable for many years, daily use of marijuana went up significantly since 2018 among eighth and 10th graders–now at 1.3% and 4.8% respectively. However, overall past year marijuana use rates remain steady among teens (35.7% among 12th graders; 28.8% among 10th graders; and 11.8% among eighth graders). Past year rates of any illicit drug use, other than marijuana, remain relatively low among 12th graders; past year use was 3.6% for LSD; 3.3% for synthetic cannabinoids; 2.2% for both cocaine and MDMA (ecstasy); and 0.4% for heroin. Other drug use, including the misuse of prescription medicines and the use of alcohol as well as tobacco cigarettes, continues to decline. "We are heartened to see the continuing decline in the use of many drugs, particularly non-medical use of prescription opioids; however, teens are clearly attracted to vaping products, which are often concentrated amounts of drugs disguised as electronic gadgets," said NIDA Director Dr. Nora Volkow. "Their growing popularity threatens to undo years of progress protecting the health of adolescents in the U.S." 12/18/2019 2 Comments Impaired DrivingThough intended to be a festive time, December often brings with it holiday-induced stressors such as facing grief and loss, increased family pressures, and finances stretched thin. Add in a surplus of social activities that commonly include alcohol, and for some during this season, staying sober can be difficult.
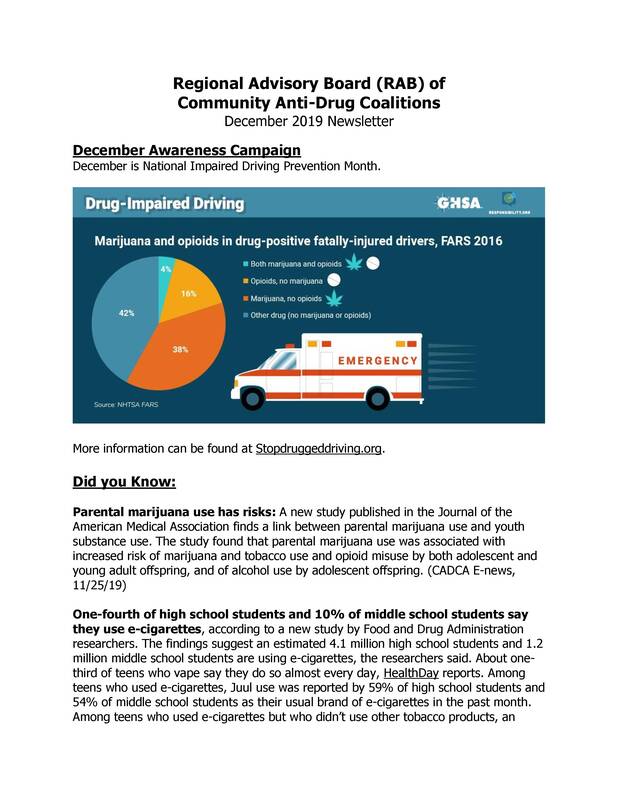
By the time New Year's Eve has come and gone, authorities see a spike in Operating While Intoxicated (OWI) offenses, binge drinking scares, and other drug- and alcohol-related issues. Buzzed Driving: The Sobering Statistics
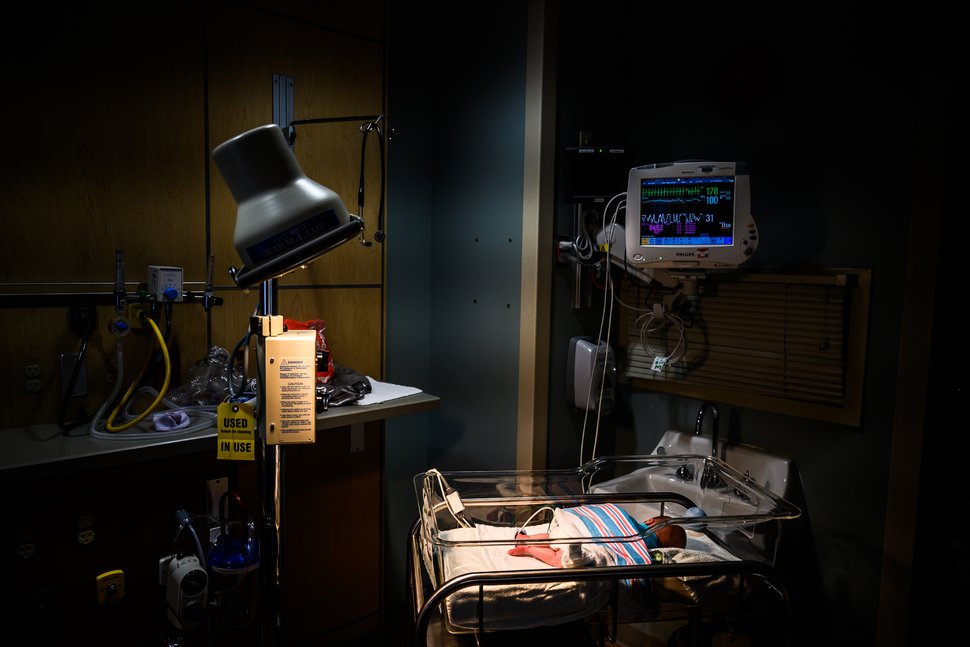
It is important to note, however, that alcohol isn’t the only substance impairing drivers—drugged driving is on the rise. Use of illicit drugs and/or the misuse of prescription drugs can also make driving a motor vehicle unsafe. According to the 2017 National Survey on Drug Use and Health, nearly 13 million people drove after using illicit drugs. As the statistics show, drinking and/or using illicit drugs and driving should never be combined. All too often people believe they are “okay to drive” when in fact they are not. Unsure how to determine if you are too impaired to drive? The bottom line is this: If You Feel Different, You Drive Different. Avoid making poor decisions at holiday events by planning ahead and ensuring a sober ride home in advance of any alcohol consumption. Help keep our roadways safe this holiday season. Plan ahead, establish safe transportation, and avoid impaired driving. Remember, driving while impaired not only puts you and your passengers in danger, but also the lives of pedestrians and other drivers and their passengers. At least 2.2 million children had been affected by the U.S. opioid crisis by 2017, with that total poised to grow and the consequences likely to be felt for years to come, a new analysis shows.
Parents' opioid use is the primary reason children are affected by the crisis – whether they're living with an addicted parent or have been removed from their home, or their parent is incarcerated or has died of an overdose – according to the report from the United Hospital Fund, a health policy nonprofit based in New York. Still, an estimated 170,000 kids had opioid use disorder themselves or had accidentally taken the drugs in recent years, the analysis says. The children of the opioid crisis are likely to incur higher expenses than others during childhood – an estimated $117.5 billion in health care, special education and child welfare spending – along with another $62.1 billion in societal costs during adulthood, the study says. Even assuming a continual downward trend in opioid use, the analysis says, there still could be 4.3 million children affected by the opioid crisis at a cost of $400 billion by 2030. "Even if we could stop the epidemic cold in its tracks today, the ripples will last long into the future," says Suzanne Brundage, the study's lead author and director of UHF's Children's Health Initiative. And while states and the federal government have spent billions of dollars to combat the opioid crisis in recent years, its effects on children and families have been "overlooked in many places," Brundage says. Across the U.S. in 2017, the analysis says there were an estimated 28 opioid-affected children per 1,000, with state-level rates ranging from 54 in West Virginia to 20 in California. The total number of opioid-affected children was highest in California, at 196,000 in 2017. These disparities reflect both the magnitude of addiction and the number of children living in a state, as well as local strategies to tackle addiction, Brundage says. For example, states where greater numbers of opioid-affected children enter foster care or live with other relatives – such as Texas and Florida – may have less robust or intentional programs aimed at keeping families intact. Living with a parent dealing with drug addiction is considered an adverse childhood experience, or ACE. A recent report from the Centers for Disease Control and Prevention found that about 61% of adults have experienced at least one ACE, while nearly 1 in 6 reported four or more types. Kids who experience a greater number of ACEs are more likely to become smokers and to be severely obese, suffer from depression and develop substance use issues of their own, according to the new analysis. On average, it says, children affected by substance use disorders experience 2.1 ACEs in their lifetimes – a significant but not "abnormally high" number, according to Brundage. "Clearly, the opioid epidemic is a generator of ACEs," Brundage says. "ACEs are a normal part of our society, unfortunately, and what we need to do is think about ways of preventing ACEs and building resilient families." Last year, President Donald Trump signed the Family First Prevention Services Act, which seeks to keep children with their parents and relatives rather than placing them in foster homes. The law enables states to use federal foster care and adoption assistance funding for mental health, substance abuse and parenting skills programs for parents at risk of losing their children. It's still unclear how the law will be implemented, though, as many states have delayed doing so. "The opioid epidemic is clearly driving forward a wave of children affected by family substance use disorder," Brundage says. "We need policymakers, (the) private sector, community leaders and the general public to … start responding today." A Town Hall Meeting to discuss Underage Drinking in Jay County will be held Thursday November 21st at 6:00PM at the Jay County Fairgrounds. If you are a parent in Jay County who would like your voice to be heard in the conversations on underage drinking, you won't want to miss this event. Supper will be provided, and everyone is welcome to attend.
This event is brought to the community by Purdue Extension and the Jay County Drug Prevention Coalition. Please contact Tonya Culp at 260-251-3259 ex. 1003 for more information. |
AuthorMultiple Authors including coalition staff, board members, and coalition members contribute to this page. Archives
March 2023
|
Location100 N. Meridian Street
Portland, Indiana 47371 |
About UsThe Jay County Drug Prevention Coalition (JCDPC) is part of the statewide network of the Indiana Commission to Combat Drug Abuse. The JCDPC is the Local Coordinating Council (LCC) for the community.
Contact UsGeneral Info:
(260) 251-3259 jcdpccontact@gmail.com Recovery Info: allyssa@jcdpc.org Prevention Info: jake@jcdpc.org |
|










 RSS Feed
RSS Feed

